
- Mouth and throat cancer can look like open sores, growths or discolored areas in the mouth.
- Oral and throat cancer is diagnosed using a biopsy.
- Imaging methods such as computed tomography, magnetic resonance imaging and positron emission tomography determine the size of the tumor and determine how far the cancer has spread.
- Treatment depends on the location, size, and extent of the spread of the tumor, and may include surgery, radiation therapy, and chemotherapy.
In 2018, an estimated 51,540 people (37,160 men and 14,380 women) contracted cancer of the mouth and throat in the United States, resulting in 10,030 deaths, mostly in men over the age of 50.
Cancers in the mouth and throat
Squamous cell carcinoma, d. H. Cancer, which develops in the cells of the squamous epithelium that lines the inside of the mouth and throat, is by far the most common cancer in the mouth. Other forms, such as verrucous carcinoma (wart carcinoma), malignant melanoma and Kaposi’s sarcoma are much rarer.
risk factors
The main risk factors for mouth and throat cancer are:
- tobacco use
- alcohol consumption
- Human papillomavirus (HPV) infection
Tobacco use causes many mouth and throat cancers. Tobacco use includes smoking cigarettes, cigars, or pipes, as well as chewing tobacco or betelpriem (a mixture of substances that contain tobacco, also known as paan) and snuff. In the United States, cigarette smoking (especially more than two packs a day) is the main risk factor for mouth and throat cancer. Cigar smoking can also increase the risk. Pipe smoking increases the risk of cancer in the lips that touch the mouthpiece. Chewing or snuff increases the risk by 50 percent of developing cancer in the cheeks, gums and inside of the lips, where the tobacco has the greatest contact.
Chronic or excessive alcohol consumption also increases the risk of mouth and throat cancer. The increase in risk is proportional to the amount of alcohol consumed. There is evidence that alcohol in mouthwash can contribute to mouth cancer if the mouthwash is used regularly for a long period of time.
The greatest risk is the combination of high alcohol and tobacco consumption , which is two to three times more likely to cause cancer than consuming a pleasure poison alone. Such combined use increases the risk of oral cancer 100 times for women and 38 times for men. The risk of throat cancer increases 30-fold. People who continue to use tobacco and alcohol after they have developed oral or throat cancer for the first time are more than twice as likely to have a second mouth and throat cancer compared to the normal population.
The HPV infection that wins as a risk factor is becoming increasingly important, causes genital warts and can infect the mouth during oral sex. The number of sexual partners and the frequency of oral sex are important risk factors. Certain strains of this virus predispose people to throat cancer and, to a lesser extent, to oral cancer. HPV infections increase the risk of throat cancer 16-fold, and HPV causes 60 percent of throat cancer.
Gender is a risk factor. About three quarters of mouth and throat cancer occur in men.
As with most cancers, the risk increases with age .
Other factors that increase the risk of oral cancer are constant irritation from sharp-edged damaged teeth, fillings, tooth decay or poorly fitting dentures (e.g. crowns and bridges). Previous head and neck x-rays, chronic candidiasis, and poor oral hygiene are also risk factors. Intense sun exposure can lead to lip cancer.
symptoms
The symptoms of mouth and throat cancer vary depending on where the cancer is located.
Oral cancer usually remains painless for a long time, but eventually causes pain as the ulcer grows. Pain is usually felt first when swallowed, like a rough throat. Those affected may have difficulty speaking. Squamous cell carcinomas in the mouth often look like open sores and grow slightly deep. The wounds may appear with flat or slightly raised red spots ( erythroplakia ) or white spots ( leukoplakia ).
Cancer tumors in the lips and other areas of the mouth often feel rock hard and are firmly attached to the underlying tissue. Most benign tumors in these areas can be moved freely. Discolored areas on the gums, tongue or oral mucosa can also be signs of cancer. An area in the mouth that has recently turned brown or dark may be melanoma. At the place where a cigarette or pipe is habitually held with the lips, a flat, brown, freckle-like stain can form (smoker’s stain).
Throat cancer usually causes throat pain, which becomes worse when swallowed, difficulty swallowing and speaking, and earache. Sometimes a “lump in the throat” is the first sign of throat cancer.
With most forms of mouth and throat cancer, symptoms eventually complicate food intake and people begin to lose weight.Erythroplakia and squamous cell carcinoma

IMAGE COURTESY OF DR. MED. DENT. JONATHAN A. SHIP.Leukoplakia and squamous cell carcinoma
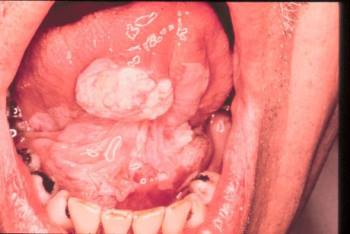
PHOTO COURTESY OF JONATHAN A. SHIP, DMD.
diagnosis
- endoscopy
- biopsy
- Imaging procedures for staging
If an abnormal area is discovered when examining the mouth and throat, the doctor will perform a biopsy (taking a tissue sample for examination under the microscope). Only a biopsy can determine whether a suspicious area is malignant. If the doctor finds abnormal growth in a patient’s mouth with symptoms, he examines the throat with a special mirror and / or a flexible viewing tube (endoscope). A biopsy of the abnormal areas identified during this examination is then performed.
If the biopsy shows cancer, the doctor z. B. Do the following imaging to determine the extent ( stage ) of the cancer:
- Computed tomography (CT)
- Magnetic resonance imaging (MRI)
- A combination of positron emission tomography (PET) and CT
These imaging studies provide the following information: size and location of the tumor, possible spread to surrounding structures, and spread to the lymph nodes in the throat. The doctor uses an endoscope to look in the mouth and throat and detect cancer in surrounding structures. These medical measures are called laryngoscopy (bronchoscopy), bronchoscopy (observation of the airways) and esophagoscopy (esophageal mirroring).
screening
Early detection significantly improves the chances of recovery. Doctors and dentists should therefore carefully check the mouth and throat area with every routine medical or dental examination. This examination must also include the area under the tongue where people will not see or feel abnormal growth until it has grown quite large.
forecast
The survival rate in people with cancer of the mouth and throat varies and depends on the following:
- Original seat of the tumor
- Spread (stage)
- root cause
The cure rate for squamous cell carcinoma in the mouth is high if the entire carcinoma and surrounding healthy tissue are removed before the lymph nodes are affected. On average, more than 75% of patients with tongue carcinoma that has not yet affected the lymph nodes live for at least 5 years after diagnosis. Approximately 75% of patients with carcinoma of the floor of the mouth that has not yet spread will survive at least 5 years after diagnosis. However, if the cancer has already affected the lymph nodes, the 5-year survival rate drops by about half. Over 90% of patients with lower lip cancer survive for at least 5 years. The carcinoma rarely spreads. Carcinoma of the upper lip tends to be more aggressive and spread.
On average, 60% of people with throat cancer survive at least the 5-year period after diagnosis. The rate is more than 75% if the human papillomavirus (HPV) is the cause, but less than 50% if the cause is something else.
Patients whose cancer is caused by HPV have a better survival rate than patients with a similar type of cancer due to other factors.
prevention
Limiting alcohol and tobacco use can significantly reduce the risk of cancer of the mouth and throat. In addition, it makes sense to have rough edges ground on damaged teeth and fillings. Avoiding direct sunlight reduces the risk of lip cancer. If the lips are largely damaged by sunburn, the outermost layer of skin can be removed surgically or with a laser to prevent cancer.
Current vaccinations against HPV target some of the strains of HPV that cause cancer of the throat. General vaccinations of children can therefore prevent the development of some of these cancers.
treatment
- surgery
- Radiotherapy, sometimes in combination with chemotherapy (chemoradiation)
The pillars of treatment for mouth and throat cancer are surgery and radiation therapy . The doctor selects the treatment based on the size and location of the tumor.
In the case of oral cancer , surgery is usually carried out as the first treatment measure. The tumor and, in some cases, the lymph nodes under and behind the jaw and along the neck are removed. Oral cancer surgery can therefore be disfiguring and trigger psychological trauma. Newer procedures in restorative surgery can improve function and restore normal appearance from the very first operation. Missing teeth and parts of the jaw can be replaced with prostheses. After extensive interventions, speech and swallowing therapies may be required. If the cancer is advanced, radiation or chemoradiation therapy is prescribed after the operation.
For patients who cannot be operated on, radiation therapy is an alternative initial treatment. Chemotherapy is not usually used as a first-line treatment, but is recommended in addition to radiation therapy for patients whose cancer has spread to many lymph nodes.
For throat cancer , surgery is more often chosen as the first treatment. Newer procedures allow doctors to operate through the mouth rather than a cut in the neck. Some procedures involve endoscopic laser surgery. In other methods, an operation robot is used. The surgeon controls the robot’s arms from the console and tracks the operation through the camera of an endoscope that has been inserted into the person’s mouth.
Radiation therapy or sometimes chemoradiation can be used either after surgery or as a first line treatment. Radiotherapy is usually used for early stage cancer and chemotherapy is used as a supplement for more advanced cancer. A special form of radiation therapy, the so-called intensity-modulated radiation therapy (IMRT), enables doctors to restrict radiation to a narrowly defined area, which can reduce side effects.
Treatment side effects
Radiotherapy of the mouth and throat causes many side effects:
- Destruction of the salivary glands, which leads to dry mouth, which in turn can cause tooth decay or other tooth problems
- Poor ability of the jawbones to heal after dental problems or injuries
- Osteoradionecrosis , loss of bone and surrounding soft tissue in the irradiated area
Because of these side effects, all existing dental problems should be completely treated before radiation therapy. Teeth that can cause problems are removed. The wounds are allowed to heal before further interventions.
Good dental care is also important for patients after radiation therapy because the mouth heals poorly after radiation exposure should dental surgery such as tooth extraction become necessary. This includes regular dental checkups and thorough daily dental care at home, including fluoride. If a tooth has to be extracted later, hyperbaric oxygen therapy can be helpful so that the jaw heals well and there is no osteoradionecrosis.